Osteoporosis is a bone disease characterized by a decrease in bone mineral density (BMD), causing structural changes that weaken bone. When viewed under a microscope, bone appears like a honeycomb – in osteoporotic bone the honeycomb spaces are more open, while the supportive lattice structures are further apart and less robust, than in healthy bone.
The (BMD) can be assessed by a special type of X-ray machine, in a procedure commonly called a DXA (Dexa) scan. The scan will generate two scores: a T-score and a Z-score. The T-score is the most important, and is a comparison of an individual’s (BMD) to that of the average bone density of a healthy 30 year old adult. How far below that average score an individual’s (BMD) is, determines if they have the diagnosis of osteoporosis. The number is a representation of how many standard deviations (SD) (statistical formula that shows distance from an average or mean) an individual is from the norm. If the T-score is -2.5 (SD) below the norm, that individual has osteoporosis. If the T-score is -1.0 to -2.4 (SD) then that individual has osteopenia (bone density lower than usual). The Z-score is a comparison of an individual’s (BMD) to that of healthy people of the same age and body type. The Z-score is more commonly used for assessing (BMD) in children, teens, and pre-menopausal women, where a comparison with their peer group is more significant.
Some of the risk factors for developing osteoporosis include: being female, family history, Caucasian or Asian, small boned frame, smoking, high alcohol intake, sedentary lifestyle, early menopause, post-menopausal, long course of corticosteroid medication, low testosterone – Men.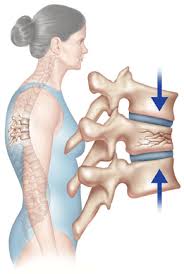
In addition to drug therapies, there is much that a person with a diagnosis of osteoporosis can do to help themselves. They must first become familiar with movements that put them at greater risk. Decreased bone density makes the bones more likely to break if too much of the wrong force is put on the skeletal structure, as with increased incidence of hip and wrist fractures from falls. Less obvious are the spinal compression fractures that can result from poor postural positioning during flexing the spine forward, as in reaching forward to pick an item off the floor. Twisting or rotating the spine is also potentially damaging to osteoporotic bone. These movements place extra force on the front side of the so called, “body” of the vertebrae, causing a crushing down in height of the affected vertebrae. Patients who suffer from a vertebral compression fracture may or may not have associated pain, and often lose height seemingly “overnight,” finding it much harder to stand up straight due to a lack of skeletal support.
Therefore people with osteoporosis should attempt to not bend forward from the waist – instead they employ a technique called hip hinging. Hip hinging keeps the spine straight (think: broom handle along your spine and back of head) as the individual leans forward keeping their chest open and their back long. This technique places less stress on the spine and more load on the legs, knees, ankles, and feet. This requires strength and flexibility in the hips, knees, and ankles. People who do not have enough of this strength and flexibility may need to use assistive devices like “reachers” and sock donners to help them with “bending over” tasks in order to not overly flex the spine.
Appropriate exercises that load bones and muscles can have a positive effect on slowing down bone loss and has potential to stimulate bone growth in some cases. There are two types of bone cells involved with bone tissue. Osteoblasts build bone and osteoclasts break down bone tissue. Whichever of these cell types is more active, determines whether bone is being built or broken down. Age, hormones (post vs. pre-menopausal status), activity levels/muscle mass, and genetics, all influence the dynamic state of bone density. Loading bones through exercises that put stress through the spine and hips can stimulate osteoblast activity, which may slow bone loss.
Weight bearing activities like walking (especially hills) and stair ascending/descending, place gravity enhanced pressure through the skeletal structure from the top down and the bottom up. For most benefit, the load needs to be transferred along an upright spine and through the hips. Walking with proper upright posture is better for loading the spine and hips. Hiking poles can assist this upright walking position, and allows force to enter through the arms and shoulders. There is evidence that doing a wide variety of weight bearing activities has a multiplied effect. It turns out that the body becomes very used to the same activity when repeated over and over. It is therefore important to “surprise your bones” with different angles and stresses. For example walking backwards or sideways or hopping. Exercises where there is less pounding of the feet on the ground, like swimming and bicycling, offer less of an advantage than walking, jogging, dancing, hopping, etc.
Building muscle mass and strength can also stimulate bone formation. Muscles attach to bones, so when a muscle contracts it places a pulling stress on the bone itself. This load then “stresses” the bone and tells the osteoblasts to become more active. Hip and core strength also contribute to balance and control during activities of daily living. Thus reducing the chance of falls even more. So with your doctor’s approval, and the supervision of a qualified medical professional, a program can be tailored to meet any individual’s needs. Much can be done to limit the effect of an osteopenia or osteoporosis diagnosis, but it starts with you.
The National Osteoporosis Foundation is a great resource for those with more questions (www.Nof.org).
We want to thank Michael Abbas, PTA at Mountain Physical Therapy for contributing this article for our newsletter. We appreciate ya!

